Revista de la Sociedad Venezolana de Microbiología
versión impresa ISSN 1315-2556
Rev. Soc. Ven. Microbiol. vol.37 no.1 Caracas jun. 2017
Auricular Chromoblastomycosis: an atypical presentation case and review of literature
Dilia Martínez-Méndeza,*, Leyla Humbría-Garcíab, Neomar Semprún-Hernándeza, Rosaura Hernández-Vallesb
a Laboratorio de Inmunología. Facultad Experimental de Ciencias. Universidad del Zulia. Venezuela. b Laboratorio de Micología. Universidad Nacional Experimental Francisco de Miranda. Venezuela.
* Correspondencia: E-mail: dmartinezmendez@hotmail.com
Abstract: Chromoblastomycosis (CBM) is a chronic, localized deep fungal infection of the skin and subcutaneous tissues, caused by dematiaceous (black) fungi. We describe the case of 62 years-old-male patient, from a rural town, with seborrheic dermatitis for more than 10 years, and a desquamative lesion in the right ear, where no diagnosis of CBM was never made. Direct exam with KOH, macro and microscopic culture characteristics, epidemiological and clinical findings confirmed the diagnosis of CBM by Cladophialophora carrionii, the first case report of auricular lesions published in Venezuela.
Keywords: chromoblastomycosis, Venezuela, auricular, Cladophialophora carrionii.
Cromoblastomicosis auricular: un caso de presentación atípica y revisión de la literatura
Resumen: La cromoblastomicosis (CBM) es una infección fúngica profunda localizada de la piel y el tejido celular subcutáneo, de evolución crónica, causada por hongos dematiáceos (negros). Se describe el caso de un paciente masculino de 62 años, proveniente de una población rural, con dermatitis seborreica por más de 10 años y una lesión descamativa en pabellón auricular derecho, donde nunca se realizó diagnóstico de CBM. Las características macro y microscópicas del cultivo, la epidemiologia y los hallazgos clínicos de la lesión confirmaron el diagnóstico de CBM por Cladophialophora carrionii, el primer caso de lesión auricular publicado en Venezuela.
Palabras clave: cromoblastomicosis, Venezuela, auricular, Cladophialophora carrionii.
Recibido 19 de enero de 2017; aceptado 5 de mayo de 2017
Introduction
Chromoblastomycosis (CBM) is a chronic, localized deep fungal infection of the skin and subcutaneous tissue, caused by dematiaceous (black) fungi, living as saprophytes on plants (Cactaceae spp.) or vegetable debris in the soil [1] All agents generate the same parasitic forms: sclerotic cells (fumagoid cells or Medlars cell scleronts) [1,2]. Clinically, the infection is characterized by a slow development, and in some cases causing irreversible deformation and partial disability of the affected limb [1,3]. CBM is not a mandatory reportable disease, so the number of cases reported by researchers and study groups summarizes the epidemiological data. The description of cases in atypical anatomical areas represents an extraordinary opportunity to update knowledge and to remind the importance of thinking about this disease to make an appropriate diagnosis. To the best of our knowledge, this is the first published report in Venezuela of auricular lesions of CBM.
Case
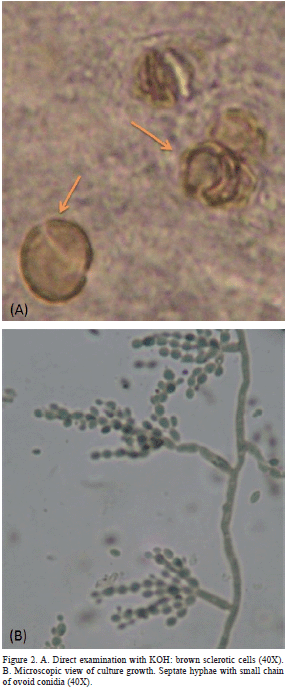
A 62-year-old-man, from Agua Larga, a rural town located at the south of the Sierra de San Luis, Falcon state of Venezuela, with symptoms of seborrheic dermatitis for more than 10 years. After physical examination, dandruff on the scalp region was find, however, the characteristics of a lesion observed on the right ear, drew significant attention. It was observe desquamative and hyperemic areas with crusts on the right ear, and areas of black dots (Figure 1). After patients acceptance through informed consent, a sample was collect by scraping the affected areas. Direct KOH examination showed several sclerotic cells (coffee beans like structures, of 4 to 10 μm, brown colored, with thick walls and septum, which could be seen single or grouped) thus confirming the clinical diagnosis (Figure 2A).
Culture on Sabouraud Dextrose Agar (SDA), incubated at room temperature (26-28 oC) after 15 days, showed velvety colonies with dark olivaceous color. Microcultures were performing on SDA at 37 oC in humid chamber, and septate hyphae with small chains of ovoid conidia were observed (Figure 2B). Direct exam with KOH, macro and microscopic culture characteristics, plus epidemiological and clinical findings confirmed the diagnosis of CBM by Cladophialophora carrionii. Strain was kept on laboratory cultures as AL-2009/UNEFM. Treatment was started with 200 mg itraconazole daily, showed improvement at the first control. However, we could not follow evolution, as he did not attend other controls.
Discussion
Chromoblastomycosis is a chronic, localized deep fungal infection of the skin and subcutaneous tissue, caused by dematiaceous (black) fungi, described over a century ago. Usually affects individuals from rural and poverty areas. Unfortunately, it is not considered a public health issue, and it is not among the priorities of national/local health systems, even in endemic countries, such as Brazil, Madagascar, Mexico, South Africa, and Venezuela. Also many cases have been described in Australia, China, Guadalupe, India, Japan, Malaysia, United States, other Latin American, and some European countries, extending the classical definition of this mycosis to tropical and subtropical areas; so CBM has a worldwide distribution [4,5]. CBM is not a mandatory reportable disease and nor does it appear in the list of neglected diseases of the World Health Organization (WHO), so the systematic reporting in the international publications have clinical and epidemiological relevance and supports case studies of working groups, which describe for each case, the typical or atypical evolution and new species involved [3].
This fungal infection usually affects asymmetrically, unilaterally and predominantly on the lower limbs, although in some countries, it involves arms and it might affect the thorax. The anatomical location of lesions has been associated with exposure to trauma during work, such as goat breeding, logging, harvesting of fruits in deciduous trees, and Cactaceae spp. farming, without the proper use of footwear protection. These observations suggest that CBM is also an occupational disease [1].
There is little data published on auricular lesions [6-10]. Iwatsu et al, reported a case of CBM that involved the auricle in a patient from Japan and the etiological agent was Fonsecaea pedrosoi [6]. Bittencourt et al, presented a case of auricular CMB mimicking an eczematous lesions and the etiologic agent was Phialophora verrucosa [7]. Arango et al, described a 60-year-old Colombian male, urban resident, who had a dark pigmented lesion, infiltrative and crusty in the ear for 5 years, caused by Rhinocladiella aquaspersa, with a good response to itraconazole therapy at a dose of 200 mg/day for 7 months [8]. França et al, reported another auricular CBM in a 67-year-old man caused by F. pedrosoi, the most common agent in Brazil [9], and Muñoz et al, presented a case located in the left ear of a 29-yearold male from Mexico, caused by F. pedrosoi, treated with itraconazole 200 mg daily for 10 weeks, with complete resolution [10].
In Venezuela, the most frequent agent of CMB is Cladophialophora carrionii, reported in semi-arid regions; however, F. pedrosoi, P. verrucosa and R. aquaspersa are also found [1,2,4]. In this work, we described an auricular lesion caused by C. carrionii. The patient was a farmer and denied having suffered trauma on the ear with a Cactaceae splinter and used a hat for sun protection. For harvesting, he used a sort of sac made of cocuiza (Furcraea andina), a rough and porous material easily allows for plants residues to adhere to the sac, that when it is placed on the right shoulder for transporting it could rub the ear. It is presumed that exposure may have occurred while performing this task, because the bag was placed on the floor, dragged short stretches where they can easily collect small pieces of plant debris containing the saprophyte phase of the fungus, becoming a rare transmission mechanism. The initial lesion should have been unnoticeable, without phlogosis signs, which slowly evolved into small scaly areas, not severe and painless, so the patient felt that the ear injured was affect by dandruff, and the CBM diagnosis was never made. The successful treatment of CBM is often unrewarding though; therapeutic response to itraconazole and terbinafine are good options in C. carrionii cases [5].
Unfortunately, the patient did not seek treatment, most likely because our hospital is not easily accessible to people living in these areas. Moreover, another situation of neglected diseases is the lack of basic, medical and logistics services near poor and rural towns.
It is very important to remember that traumatic infection by the agent does not always has the classic presentations in limbs, therefore it is necessary to investigate clinical, microscopic and eco-epidemiological areas.
Acknowledgements
To Jesús Esquivel, Dee Cocheran and Cristóbal Grau, for critically review of the manuscript.
Conflicts of interest
The authors declare no conflict of interest.
References
1. Yegres F, Richard-Yegres N. Cladophialophora carrionii: aportes al conocimiento de la endemia en Venezuela durante el siglo XX. Rev Soc Ven Microbiol. 2002; 22:153-7. [ Links ]
2. Pérez-Blanco M, Fernández-Zeppenfeldt G, Hernández R, Yegres F, Borelli D. Cromomicosis por Rhinocladiella aquaspera: primer caso en Venezuela. Rev Iberoam Micol. 1998; 15:51-4. [ Links ]
3. Queiroz-Telles F. Chromoblastomycosis: a neglected tropical disease. Rev Inst Med Trop Sao Paulo. 2015; 57(Suppl 19):S46-50. [ Links ]
4. Martínez Méndez D, Hernández Valles R, Alvarado P, Mendoza M. Las micosis en Venezuela: casuística de los Grupos de Trabajo en Micología (1984-2010). Ver Iberoam Micol. 2013; 30:39-46. [ Links ]
5. Esterre P, Andriantsimahavandy A, Ramarcel ER, Pecarrere JL. Forty years of chromoblastomycosis in Madagascar: a review. Am J Trop Med Hyg. 1996; 55: 45-7. [ Links ]
6. Iwatsu T, Takano M, Okamoto S. Auricular chromomycosis. Arch Dermatol. 1983; 119:88-9. [ Links ]
7. Bittencourt AL, Londero AT, Andrade JA. Auricular chromoblastomycosis. A case report. Rev Inst Med Trop Sao Paulo. 1994; 36:381-3. [ Links ]
8. Arango M, Jaramillo C, Cortés A, Restrepo A. Auricular chromoblastomycosis caused by Rhinocladiella aquaspersa. Med Mycol. 1998; 36:43-5. [ Links ]
9. França K, Villa RT, Bastos VR, Almeida AC, Massucatti K, Fukumaru D, Bedin V. Auricular chromoblastomycosis: a case report and review of published literature. Mycopathologia 2011; 172:69-72. [ Links ]
10. Muñoz Estrada VF, Valenzuela Paz G, Rochín Tolosa M. Cromomicosis: reporte de un caso con topografía atípica. Rev Iberoam Micol. 2011; 28:50-2. [ Links ]












 uBio
uBio